News Article
Intraocular pressure (IOP) is a key risk factor for glaucoma, one of the leading causes of irreversible vision loss. Traditionally, IOP testing only happened during office visits. Unfortunately, that only provides a brief glimpse of a patient’s eye pressure at a time. IOP levels fluctuate throughout the day, and these changes can impact disease progression.
However, home tonometry transforms glaucoma management, allowing patients to conduct IOP testing in real-time. Devices such as the iCare HOME2 tonometer and contact lens sensors make it simple to monitor eye pressure. They are noninvasive and user-friendly. Learn more about what a tonometer is.
This shift from clinic-based testing to home monitoring empowers patients to take a more active role in their treatment, thereby enhancing early detection, improving medication adherence, and promoting long-term outcomes.
IOP plays a critical role in eye health, particularly in the management of glaucoma. Elevated IOP is a significant risk factor for glaucoma, which can lead to blindness without appropriate management. Traditional IOP testing happens at a doctor’s office, but these single readings don’t always capture the complete picture.
IOP levels fluctuate throughout the day. But what if a pressure spike doesn’t coincide with an office visit? That’s valuable insight that could affect your treatment.
Enter at-home IOP tests. A handheld tonometer, also known as an eye pressure meter, enables patients to monitor fluctuations in intraocular pressure. Most importantly, they can provide real-time data to their doctors, supporting and improving glaucoma management.
Tonometry devices give patients control of their eye health in ways that were once only possible in a clinic.
At-home IOP monitoring is changing how patients manage their eye health. Patients can track their eye pressure measurements regularly using portable devices, such as handheld tonometers, and share the data with their doctors. This real-time insight enables the early detection of elevated IOP, facilitates more effective treatment adjustments, and promotes improved medication adherence.
Beyond convenience, at-home monitoring helps reduce unnecessary clinic visits. Let’s explore how these benefits are reshaping glaucoma management:
IOP refers to the pressure inside the eye, measured in millimeters of mercury (mmHg). A normal range falls between 10 and 21 mmHg, with 20 mmHg often used as a general threshold for concern.
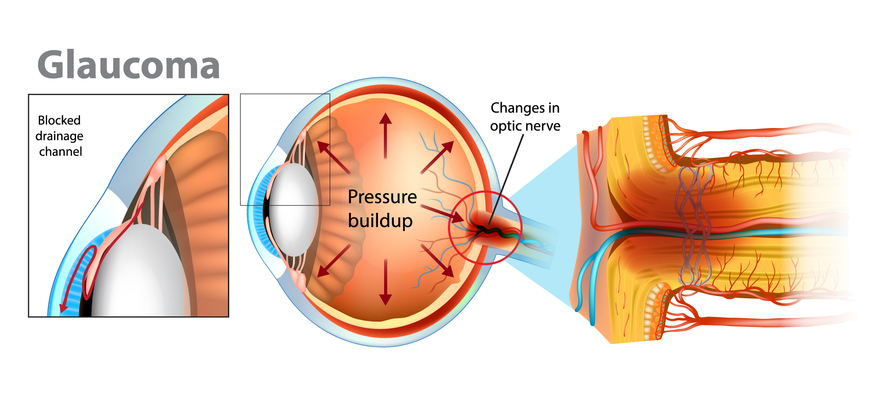
The aqueous humor, the fluid that nourishes the eye and maintains its shape, affects intraocular pressure. When aqueous humor fails to drain properly, pressure builds up, resulting in elevated IOP. Over time, this can damage the optic nerve, increasing the risk of glaucoma. IOP testing enables the detection of elevated pressure.
Factors that cause fluctuation in IOP include:
Please note that these factors fluctuate on a daily basis. Therefore, a single eye pressure measurement taken during an office visit may not accurately reflect a patient’s risk. That’s why frequent monitoring at home can be life-changing for people with ocular hypertension or glaucoma.
Traditionally, IOP measurements involve various types of tonometry. The most common methods include:
While Goldmann Applanation Tonometry is the most precise method, rebound tonometry has made home monitoring practical and accurate.

A home tonometry device provides patients with real-time IOP measurements, eliminating the need for a trip to the clinic. Devices like the iCare HOME2 tonometer have easily made it possible for patients to monitor their eye pressure. Moreover, companies like MyEyes make renting or buying their at-home tonometer simple.
Technology is making at-home IOP testing even more advanced and accessible. Future innovations include:
With these advancements, patients will gain even greater control over their eye health.
IOP testing is a key factor in glaucoma management. Handheld tonometers, such as the iCare HOME2, allow you to take IOP measurements from the comfort of your own home. Discover how to rent or purchase a home tonometer.
Remember, consistent at-home IOP measurements help detect fluctuations in IOP, which improves treatment and reduces the risk of vision loss. Change the way you manage your glaucoma to preserve your vision!

Our mission is to make it easier to get home tonometers into hands of the people who need it. In this way, IOP data collected at home at various time points during the day and or night can help to direct an individual patients’ doctors to provide the ideal treatment for that patient’s tailored need.
Hear from glaucoma and industry experts sharing insights on the latest trending topics that are shaping glaucoma.