News Article
Glaucoma is a group of eye diseases that can lead to blindness if left untreated. It occurs when high pressure in the eye, known as intraocular pressure (IOP), damages the optic nerve, which is essential for good vision.
Often referred to as the “silent thief of sight,” the disease progresses slowly and may not exhibit symptoms in its early stages. However, with early detection and proper care, vision loss can be minimized or prevented.
Glaucoma is a condition in which increased eye pressure damages the optic nerve. The optic nerve carries visual signals from the eye to the brain, and any damage can result in vision loss. Indeed, the disease is a leading cause of blindness.
While high intraocular pressure is the most common cause, glaucoma can also occur with normal IOP pressure.
There are several types of glaucoma:
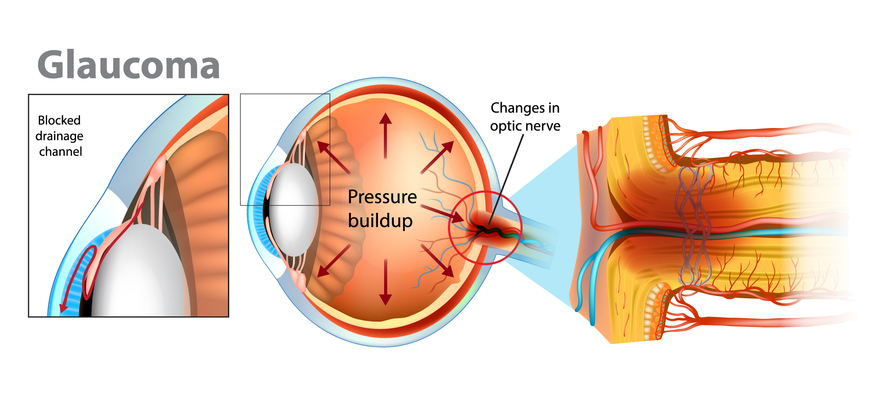
Glaucoma is often caused by increased eye pressure, which happens when the eye’s drainage system doesn’t function properly. Other factors can also contribute, such as:
If you have these risk factors, regular visits to your eye doctor are critical for early detection.
One challenge of managing this condition is that it often has no early symptoms. This is especially true for the primary open-angle type. However, as the disease progresses, signs may appear, including:
In contrast, acute angle-closure glaucoma has more immediate and severe symptoms:
If you notice these symptoms, consult an eye doctor immediately.
Early detection is key to managing glaucoma effectively. Regular eye exams are crucial, especially for individuals at a higher risk. During an exam, your eye doctor may use several tests to check for signs, including:
For people diagnosed with this condition, regular eye pressure tests are crucial. Fortunately, using a tonometer, self-tonometry enables you to track your eye pressure from the comfort of your own home.
This empowers you to participate actively in treatment planning and ensures prompt response to changes in pressure inside the eye.
Treating glaucoma focuses on lowering eye pressure to prevent further damage to the optic nerve. Treatment options vary based on the type and severity of the condition.
Most patients begin with medicated eye drops. They help reduce high eye pressure by decreasing fluid production or improving fluid drainage. Common types include:
Taking these drops consistently is vital for effective glaucoma care.

Laser treatments can improve fluid drainage or reduce fluid production. For example:
If medications and laser therapy are not sufficient, surgery may be necessary:
New therapies are being developed to improve glaucoma care. Minimally invasive glaucoma surgeries (MIGS) are less invasive and have faster recovery times. Additionally, research into neuroprotective treatments and genetic therapies holds promise for better outcomes.
Monitoring intraocular pressure (IOP) is critical to managing glaucoma and preventing further damage to the optic nerve. Traditionally, patients visit their eye doctor regularly to measure the pressure inside their eyes.
However, advancements in technology now allow for self-tonometry. It enables you to measure IOP accurately from the comfort of your own home using a handheld tonometer.
Self-tonometry involves using a compact, easy-to-use device called a tonometer (what is a tonometer) to monitor IOP. Tools like the iCare HOME2 tonometer from MyEyes enable patients to track changes in eye pressure conveniently.
You can measure and record your IOP levels with just a few simple steps. More importantly, you can give your eye doctor valuable data for treatment planning and early intervention.
Self-tonometry is particularly beneficial for individuals with glaucoma or those at high risk of developing it. Here’s why:

Home tonometry substantially advances glaucoma care. Best of all, the process is simple:
Managing glaucoma requires a proactive approach. Here are some tips:
While you can’t always prevent glaucoma, you can reduce your risk with these steps:
Proactive care is your best defense against damage to the optic nerve caused by high eye pressure.
Glaucoma is a serious eye condition, but early detection and proper treatment can help preserve your vision. From medications to surgeries, glaucoma treatment options focus on controlling IOP and preventing further damage to the optic nerve.
Tools like the MyEyes in-home tonometer make it easier to stay on top of your glaucoma care. You can purchase or rent the device. You’ll also access live customer support to help you learn how to use the ocular tonometer.
Don’t wait until symptoms appear. Schedule an eye exam today, or explore how the HOME2 tonometer can support your glaucoma care journey. Protect your vision—your future self will thank you.

Our mission is to make it easier to get home tonometers into hands of the people who need it. In this way, IOP data collected at home at various time points during the day and or night can help to direct an individual patients’ doctors to provide the ideal treatment for that patient’s tailored need.
Hear from glaucoma and industry experts sharing insights on the latest trending topics that are shaping glaucoma.